Our Mission
Through the Open Aortic Surgery Foundation Fund (“ASFF”), a 501(c)(4) foundation, we seek to provide Post-Residency / Fellowship Surgical Trainees and Operative Advanced Practice Providers (“Surgical APPs”) with a unique Super Fellowship opportunity to train in Open Aortic Surgery at top institutions with the hope of improving surgical outcomes for patients impacted by Connective Tissue Disorders.
We are selecting a Pilot Academic Institution and Pilot Institution Surgical Director to facilitate surgical mentorship, operative experience, surgical research and enhanced expertise to provide open aortic operative care for these vulnerable patients.
The Need
With an increased focus on endovascular techniques to treat aortic aneurysms, connective tissue patients are finding increasingly limited options in finding experts trained in traditional Open Aortic Surgery for long-term durable solutions.
The Open Aortic Surgery “Super Fellowship”
What is a Super Fellowship?
After completing traditional fellowship or integrated residency in cardiothoracic (CT) or vascular surgery, many trainees spend time in non-accredited “super fellowships”.
The reasons for further instruction are varied, but relate to readiness and need for specialized skills.
As surgical training has focused increasingly on “minimally invasive” procedures, Cardiovascular Surgeons are losing operative exposure to large, open procedures which require an increasing amount of technical skill. Patients with connective tissue pathology are best suited for traditional open surgery to address issues with critical anatomy, specifically the aorta. This has resulted in a disproportionate volume of cases at a select number of institutions.
We believe that this concentration of volume has created a ‘monopolistic complex’ that serves those few institutions well, but has not meaningfully helped these patients by providing them options for high-risk surgical care.
What can ASFF do about this?
It is quite simple. We can fund experience! We seek to create additional centers with the requisite surgeons who can perform these highly-complex open aortic surgeries by providing “super fellowship” opportunities in this area of cardiovascular surgery.
After selection of a Pilot Institution and Pilot Institution Surgical Director, the ASFF will begin funding elite surgical trainees as the inaugural call of the Open Aortic Surgery Super Fellowship.
The Pilot Institution
We are actively seeking a “Pilot Institution” that will help create a Super Fellowship using ASFF’s funding. The Pilot Institution will have a young director who has either Cardiothroracic / Vascular surgical training from top institutions who is passionate about providing future trainees with Open Aortic surgery training.
Pilot Institution Surgical Director
We are seeking a young attending Cardiothoracic or Vascular Surgeon who will serve as the Pilot Super Fellowship director, in addition to his / her academic and clinical practice. We want a young surgeon to set a tone that the days of the monopoly on open aortic surgery are over. A young, talented surgeon will have a unique opportunity to create an enduring legacy as the inaugural Surgical Super Fellowship Director.
Pilot Institution Surgical Director Compensation
The Pilot Institution Surgical Director will receive an annual compensation grant of $150,000 to oversee the Super Fellowship program at his / her institution. The compensation grant will be for a 2-year period ($300,000 total), and will be subject to renewal on a bi-annual period by the Foundation’s Board of Trustees.
We will begin accepting applications for this role in March-2025. The application and selection process is being developed and will be available shortly.
Developing how it works.
The ASFF Surgical APP Aortic Fellowship Grant
Advanced Practitioner Providers as essential hands in the Open Aortic Operative Field
APPs have long played a role in the intraoperative phase of major surgery. Most open heart cases in the U.S. have a Physician Assistant (“PA”) or Advance Practice Registered Nurse with a First Assistant certification (“APRN / DNP RNFA”) scrubbed in the case. The range in the level of autonomy afforded APPs during the intraoperative period is largely based on the APP’s technical skill set, the type of institution where the surgery is being performed (academic v. non-academic) and most importantly, the level of comfort that the lead attending surgeon has with the APP. In some instances, the APP will function at a level equivalent to a “co-surgeon” whereas others may be limited to more support functions (prepping / draping, retracting, etc.).
Operative efficacy & continuity: What has long been missing is understanding the value that APPs bring to operative efficacy. APPs, unlike residents and fellows, do not rotate nor have a set timeline. This enables a significant return on investment for those that find surgeons willing to spend the extra time to train and reinforce the mentality that “excellence is the expectation and not the aspiration”.
Continuum-of-care: The idea of a provider with involvement in the whole process has many benefits. For patients, most find it incredibly comforting to have someone scrubbed-in on their cases who are part of the entire surgical process - from intake to consultation to planning to surgery and eventually to discharge. For instance, if closing an aorta post AVR and the aortic tissue is particularly fragile, the APP will know that post-op blood pressure management will be even more critical to monitor. If a different practitioner had been operating, that concern may not be communicated adequately even in a robust ‘hand-off’ protocol. The surgeon who practices with an APP First Assistant can feel at ease knowing that both his or her needs and the patients’ needs will be met. The APP who is familiar with the patient will know just what the surgeon will want in the operating room, will have appropriate equipment, supplies, support staff etc available, therefore making the patients’ surgical experience smooth and uneventful. A first assistant that does not have that relationship with the surgeon or patient cannot offer those intangible benefits. Ideally, the best ‘surgical assistants*’ would be patient care roles that encompassed the entire patient surgical experience from pre-operative evaluation to patient discharge, which is the spectrum of both APRN RNFAs and PAs.
An Enduring Legacy
The Foundation’s Benefactor is a Marfan Syndrome patient. Diagnosed at age 12, he fights the disease and has endured major open aortic surgical intervention. He has suffered immensely but has fought the disease and undergone some of the biggest open aortic surgeries suffering death-defying complications along the way:
In February-2016, he underwent an Open Extent II Thoracoabdominal Aortic Aneurysm repair - a surgery that was described as ‘cutting the body in half’ to access the entire aorta in order to replace both the ascending and descending diseased portions with a Dacron graft. During surgery, he suffered an Acute MI and required open cardiac massage to restart his heart. Short video clip of the heroic Surgical PA who massaged the heart for nearly 15 min.
In January-2020, he underwent what many called the largest cardiovascular surgery performed in modern medicine when he had his second Open Extent II Thoracoabdominal Aortic Aneurysm repair, combined with a Subtotal Esophagectomy to repair an Aortoesophageal Fistula. This case received much attention in the academic cardiothoracic community and was presented as a case study. For over 20 hours, with over 40 people in the room, the team showed heroic expertise that has only been achieved a handful of times in the surgical literature.
“Unfortunately, Open Thoracoabdominal Repairs are ‘maximally-invasive’. The best description as I can give (as crude as it is) is popping open the body like a Pillsbury dough can. Accessing the entire aorta is an endeavor of epic proportion - we have to cut the body in half to access the aorta behind critical anatomy.”
‘Count Back from 10’
A story of Marfan Syndrome through the eyes of a patient enduring epic life-saving surgeries and the heroes who have devoted their lives to developing heroic surgical expertise.
-
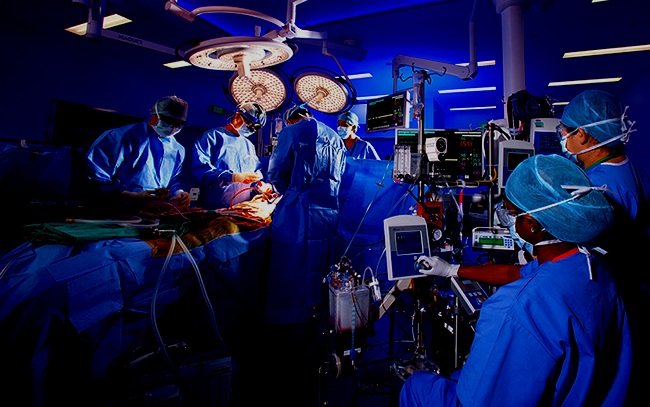
The date was January 17, 2020 - a Friday like none other. I exchange "see you later" with my family in the holding area and I am wheeled into a large Operating Room. I become the center of attention for a large team all geared up and setting the room for their performance. I once read that Operating Rooms were called "theaters". I see how that connection was drawn. The team is wearing costumes - not for show but for function. All are wearing teal-colored scrubs, some have already 'gloved-and-gowned', a well-rehearsed sequence between the nurses and those that will be on center-stage (in the "operative field" as they call it). A few are wearing telescopic loupes and headlights to visualize my the most intricate areas of my anatomy.
The Anesthesiologist, a young woman with a calming voice, puts the mask over my mouth and as she holds my hand, asks me to count back from 10. My first role in the theater of Cardiac Surgery has begun. Ten hours later, I am in the Cardiac Intensive Care Unit. Days later, I learn that the Perfusionist had me under Deep Hypothermic Circulatory Arrest (DHCA) for over 70 minutes as my drama unfolded.
I also learn of the heroics of the Physician Assistant who manually massaged my heart for 15 minutes after it stopped as the surgeon was nearly finished wiring my sternum back together.
My surgical journey with the insidious Marfan Syndrome had officially begun. As I now face the 'mother of all cardiac surgeries' - an open repair of a thoracoabdominal aortic aneurysm, I reflect on a journey of hope, despair and the heroes who dare to perform on the most intense stage of all.
These are the stories of my journey from the brink of death and all the heroes who have dedicated their lives to Cardiac Surgery.
-
Every surgeon and surgical APP who performs these incredibly invasive surgeries has stories to tell - stories of hope, heartbreak, and heroics. Patients facing these surgeries deserve to hear them all.









